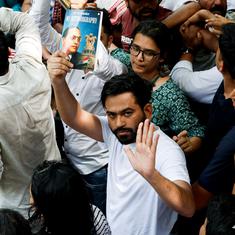On Wednesday, almost 2.7 lakh Indian doctors protested the National Medical Commission Bill, 2016 by holding dharnas across the country. Drafted by the government planning body NITI Aayog, the bill aims to create a “world class medical-education system” by replacing the Medical Council of India with a new National Medical Commission.
World Medical Association, an international organisation representing physicians globally, has supported the Indian Medical Association’s protest against the move. The Indian Medical Association is a member of the World Medical Association.
The Medical Council of India, a statutory body, is primarily responsible for recognising medical colleges and registering doctors allowing them to practice. The body was marred with allegations of corruption. Former Union Health Minister Dr Harsh Vardhan had publicly stated that the council is corrupt and needs reforms. Former president of the council Dr Ketan Desai was arrested by the Central Bureau of Investigation for allegedly accepting a bribe of Rs 2 crore from a medical college in Punjab. Desai has also headed the Indian Medical Association in the past and was recently appointed president of the World Medical Association. The Indian Medical Association itself has been criticised in the past for endorsing commercial products.
A committee for the reform of the Indian Medical Council Act, 1956 was set up by the government in March this year, which suggested the formation of the National Medical Commission through a new Act of Parliament.
The Indian Medical Association has labelled the bill draconian as it allows for non-medics to become a part of the highest ethical body of doctors in India. “Under the proposed Act, babus sitting in air-conditioned offices will decide what a doctor should do,” said Dr S Utture, a former elected member of Maharashtra Medical Council, which looks at registering of allopathic doctors in Maharashtra and is a quasi-judicial body responsible for hearing cases of medical negligence. Unlike Medical Council of India, the state council like Maharashtra Medical Council have nominee from the state government.
Undemocratic commission
Utture and his colleagues at the Indian Medical Association believe that through the bill the government is showing its intention of allowing the inclusion of non-medics to decide how medicine should be practiced in India. “Can a doctor teach ethics to a lawyer? Then why should doctors learn anything from lawyers or architects?” asked Utture who led the protest in Maharashtra.
The National Medical Commission under the proposed act will have 20 members, including 10 part-time members. Four members will be nominated by various ministries in the union government, which doctors said is undemocratic. “Currently doctors are elected to the Medical Council of India through elections among the medical fraternity,” said Dr Jayesh Lele, member of Indian Medical Association in Mumbai. “By nominating members to the council, the government is ensuring that its own representatives enter the council who are politically controlled.”
The committee has said in its report that the current process of forming the Council creates an ab-initio – from the beginning – conflict of interest and therefore this system must be discarded in favour of one based on search and selection. Critics of the Medical Council of India’s election method said that doctors who are particularly interested in standing for elections are always appointed and doctors with calibre and expertise are not.
Former health secretary K Sujatha Rao said that doctors have to understand that the National Medical Commission is a regulatory body and not an association like the Indian Medical Association where selecting members by election is understandable. “A committee of an association can be elected but a regulatory body’s committee needs to be nominated. There is no doubt that the nomination process, however, should be a transparent one,” said Rao.
Medical education for the rich
The draft bill permits the opening of medical colleges for profit. Currently, medical colleges can be started by trusts and charitable institutes and are classified as non-profit institutes. The rationale behind the move is to address the problem of doctor shortage. The report of the reform committee said the current ban on for-profit institutions has not prevented private and supposedly non-profit institutions from extracting profits through non-transparent and possibly illegal means.
Opening medical education to private commercial players has not gone down well with many working in the field. Ironically, the Indian Medical Association has no problem with commercialisation of medical education. “As long as there is transparency with respect to fees, we will support private medical colleges,” said Dr KK Aggarwal, president of the Indian Medical Association.
Rao, who has closely studied the United States model of medical education that India seems to be following, said that increasing the number of medical colleges alone will not provide more doctors in the community. “Where will you get the teaching faculty from?” asked Rao. “The medical colleges operating in the country don’t have enough faculty. Medicine is not a math test and more colleges does not mean more quality doctors.”
Public health expert Anant Bhan believes that for-profit private medical colleges will only make medical education a distant dream for students belonging to the economically weaker sections of the country.
To ensure the quality of doctors passing out from such for-profit medical colleges, the bill proposes a National Licentiate Examination. “A multiple-choice question test cannot determine how good a doctor is. We will have to see whether they can record blood pressure also,” said Rao.
Utture said that such exams will only dissuade students from becoming doctors.
Inclusion of AYUSH doctors
The draft bill includes a fourth schedule that will allow the registration of doctors practicing ayurveda, yoga and naturopathy, unani, siddha and homeopathy – abbreviated as AYUSH – with the National Medical Commission. “The government is trying to give a back-door entry to these doctors by registering them with the council meant for allopathic doctors,” alleged Utture.
Some states like Maharashtra are considering offering courses in pharmacology to homeopathy doctors so they can prescribe allopathic drugs too. “No government is going to allow cross-pathy but if a doctor is certified to prescribe allopathic drugs then I don’t see why anyone should have a problem with it,” said Rao. Cross-pathy refers to a medic prescribing medicines that are used in a medical discipline he is not trained in, like an allopathic doctor prescribing ayurvedic remedies.
Public health experts said if the problem with commercialisation of education and transparency in the nomination of members to the council is not addressed, the draft bill will only give birth to another tainted body.